Sexuality, Intimacy and Cancer
Overcoming specific challenges
Many of the challenges in this section are common for anyone with cancer. Other challenges are less common, or caused only by particular treatments. Some changes are temporary, while others are ongoing.
Tips for managing some of the side effects of treatment and other challenges are below.
Fatigue
It’s common to feel tired and lack energy during and after cancer treatment. This can continue for weeks or months, and varies from person to person. You may lose interest in sex or need to take a less active role. Your partner may be tired, which can impact their libido.
Tips for managing fatigue
- Regular light to moderate exercise has been shown to reduce fatigue. Even a walk around the block can help. An exercise physiologist or physiotherapist can suggest exercises that are right for you.
- Plan ahead. Rest before having sex.
- Use memories and fantasies, or erotic material to spark your interest.
- Try to be intimate at different times of the day.
- Speak to an occupational therapist, cancer support nurse or a Cancer Council 13 11 20 consultant about ways to manage fatigue.
- Spend time being affectionate with your partner – hugging, kissing and holding hands are all ways of feeling close when you’re too tired for sex.
Anxiety
Feeling anxious and scared is a normal reaction to finding out that you have cancer and going through treatment. Thinking about intimacy or having sex may also make you feel anxious. You may worry about how you look, how your partner will respond or how your body will perform, dread being touched, or fear that sex will be painful. If you’re single, you may also feel worried about starting a new relationship.
Anxiety may affect your self-esteem and as a result you may lose interest in sex or find yourself avoiding it. You may feel less anxious if you find out more about your cancer and ask your treatment team what to expect. Think about how you have managed stressful situations in the past, and discuss these strategies with your partner or a trusted family member or friend.
Tips for managing anxiety
- Try mindfulness techniques, relaxation or meditation. Relaxing your body and mind often helps you feel more in control and able to cope with fear, tension and anxiety. Cancer Council has relaxation and meditation tracks available in our Finding Calm During Cancer podcast series.
- If your thoughts are unhelpful or hard to control, consider cognitive behaviour therapy (CBT). This can show you how to change thought patterns that might be getting in the way of a fulfilling sex life. A psychologist or counsellor can help. Ask your GP for a referral – you may be eligible for a Medicare rebate.
- Share your thoughts with your partner. It shows trust and helps create intimacy.
- Talk to your doctor about whether medicine may help manage your anxiety. However, some medicines may lower your libido.
How to deal with feelings of sadness and depression
It’s natural to feel down during any stage of a cancer diagnosis. Changes to your body can be upsetting and it takes time to adjust. Some medicines and treatments can also affect your mood. Simple daily habits and the tips below may help improve how you feel. Sometimes feelings of sadness become very strong, and start to affect other parts of your life, including sexuality. Talk to your treatment team if you are feeling more low than usual or if it persists.
Aim for a good night’s sleep – Poor sleep can make depression worse, so try to get up and go to bed at the same time each day. Avoid long naps or caffeine after lunchtime. In the evening, swap screen-time – watching TV or using your phone/tablet – for relaxation exercises. If you wake to go to the toilet a lot, try drinking less at night or ask your doctor if there is anything that can help.
Add an activity to your day – Getting back into activities can lift your mood. You could make a list of things you enjoyed before cancer and try one a day. Plan a time for hobbies or talking to friends, instead of waiting until you feel “up to it”. You may need to adapt – if you can’t manage a book, try an audiobook. Focus on things that make you feel good (a fun movie), or in control (finishing a job you put off). Break tasks into steps if you feel overwhelmed. If you don’t get to it today, try again tomorrow.
Eat a balanced diet – Nutritious food can help to improve your energy levels, sexuality and sleeping patterns. If you find that you don’t feel like eating anything, try a small snack until your appetite returns. Try to drink enough fluids to stay hydrated – tea, water and low-sugar juices are good choices.
Try to eat mostly healthy options with the odd treat.
Try regular exercise – Physical activity can help improve your mood, so be active if possible. Plan some exercise each day, but be kind to yourself if you can’t make it. Start slowly – if you can’t go for a walk, just be outside. Begin moving around, even if you’re not in the mood. You can always stop if you don’t feel up to it. A massage (if appropriate for your cancer type) may help you feel like being active again.
Ask about medication – Depression is common if you have low levels of sex hormones or hormone changes. Ask your doctor if your medicine or treatment could also affect your mood, sleep or libido. If you have continued feelings of depression, talk to your doctor, as counselling or medicines – even for a short time – may help. Let them know if sex is important, as some antidepressants can affect sexual function.
Where to get more help – If you worry that you, or someone you care for, may be depressed, you’ll find a checklist and helpful information by calling 1300 22 4636 or visiting Beyond Blue. For 24-hour crisis support, visit Lifeline or call 13 11 14. You can also talk to your GP or your cancer care team. In an emergency call Triple Zero (000) or go to an emergency department.
Loss of desire
While loss of desire may not be a problem for some people, changes in sex drive or interest (low libido) are common during cancer treatment.
There are many reasons why your libido might change, including:
- treatment side effects such as feeling tired and sick
- pain when recovering from surgery
- being too worried about the cancer to think about sex
- fear of pain during penetrative sex
- changes in your hormone levels
- loss of confidence and self-esteem as treatment may have changed the way you look.
Most people find that their libido returns when treatment ends, but keep in mind that hormone levels also change with age, and you may notice a gradual decrease in your sex drive as you get older.
Adjusting to changes in sex drive can be emotionally and physically challenging for people with cancer. Discuss the changes with your partner, so they can understand instead of feeling rejected.
If you feel you need further support or ideas on how to help your relationship get through this stressful time, consider talking to a counsellor, sexual health physician or sex therapist. Speak to your doctor for contacts in your local area or call Cancer Council 13 11 20.
Tips for when your libido is low
- Make it a priority to spend time with your partner. Arrange a “date” or even a weekend away.
- Enjoy physical contact without sexual penetration to maintain intimacy. Try skin-to-skin touch, such as massaging each other, or having a bath together.
- Suggest a quick, gentle lovemaking session rather than a long session.
- Keep an open mind. You could read an erotic story, watch an erotic movie or try some adult products (e.g. personal lubricants and sex toys like vibrators). These may help spark your interest in sex or your partner can masturbate, either alone or with you present.
- Stimulate yourself so you become aware of how you like to be touched.
- Change the venue. If you and your partner have been coping with the side effects of treatment at home, book a night away or try using rooms in the house that are not associated with cancer.
- If your usual sexual positions have become uncomfortable, experiment with different ones to find something that feels better.
- Use cushions or pillows to support your weight.
- Rearrange the bedroom furniture or think about redecorating once your treatment is over.
- Ask your doctor about having a hormonal assessment to check your hormone levels.
- Try different ways of getting in the mood for intimacy: wear clothes that make you feel sensual, light candles and play soothing music, shower or bathe together, share erotic images or stories, or have a weekend away if you can – whatever makes you feel sexy, relaxed and good about each other.
Ways to improve erections
There are several options for trying to improve the quality of your erections, regardless of the type of cancer treatment you have had. Ask your treatment team for more details about these methods and other things you can do to get erections firm enough for penetration.
Tablets – There are medicines used to increase blood flow to the penis. These only help if the nerves controlling erections are working. These tablets should not be taken with some blood pressure medicines. Check with your doctor if these could be suitable for you.
Your doctor may recommend using the tablets before and soon after surgery, as the increased blood flow can help preserve penis health until the nerves recover. Tablets are also an option after radiation therapy and ADT.
Vacuum erection device (VED) – A VED or “penis pump” uses suction to make blood flow into the penis. This device can also help to strengthen or maintain a natural erection. You place a clear, rigid tube over the penis. A battery-operated or manual pump then creates a vacuum that causes blood to flow into the penis so it gets hard. You place a rubber ring at the base of the penis to keep the erection firm for intercourse after the pump is removed. The ring can be worn comfortably for 30 minutes.
Talk to your doctor about suitable devices for you and where to buy them.
Penile injection therapy (PIT) – PIT involves injecting the penis with medicine that makes blood vessels in the penis expand and fill with blood, creating an erection. This usually occurs within 15 minutes and lasts for 30–60 minutes.
The medicine has to be prescribed by a doctor. It often comes in pre-loaded syringes, which are single use. You can also buy it in vials from a compounding pharmacy and measure it out into a syringe yourself.
You will be taught how to inject the penis. Injecting your penis may sound unpleasant, but many people say it causes only a moment of discomfort.
PIT works well for many people, but a few may have pain and scarring. A rare side effect is a prolonged and painful erection (known as priapism). This needs emergency medical attention.
Implants – A penile prosthesis is a permanent implant that allows you to create an erection. Flexible rods or thin, inflatable cylinders are placed in the penis during surgery and connected to a pump in the scrotum. You turn on or squeeze the pump when you want an erection.
It is usually recommended to wait at least a year after most cancer treatments before having an implant. Non-surgical options such as oral medicines or injections will usually be tried first.
Occasionally, penile implants need to be removed. If this happens, you will no longer be able to have an erection.
You may see or hear ads for ways to treat erection problems. These ads may be for herbal preparations, natural therapies, nasal sprays and lozenges. If you are thinking about using these products, talk to your doctor first, as there could be risks without any benefits. Products that contain testosterone or act like testosterone in the body may encourage some cancers to grow.
Changes in ejaculation
After surgery for prostate cancer, you will not produce semen. This means that you will have a dry orgasm, which can feel quite different – some people say it does not feel as strong or long-lasting as an orgasm with semen, while others say it is more intense. Sometimes surgery causes semen to go backwards into the bladder, rather than forwards out of the penis. This is called retrograde ejaculation. This is not dangerous or harmful, but it does mean you will be infertile.
In some cases after prostate surgery, you may leak a small amount of urine during ejaculation (this is not harmful). If you are feeling anxious about your sex life, premature ejaculation can also be a problem.
Tips for adapting to ejaculation changes
- Discuss the changes with your partner and reassure them that it doesn’t affect your enjoyment of sex. Include lots of foreplay to increase your satisfaction.
- Empty your bladder (urinate) before sex to minimise urine leakage. If you or your partner are worried, you can use a condom or constriction ring (available from sex shops) at the base of the penis to catch any leakage. Pelvic floor exercises can help improve bladder control.
- Ask your doctor about medicines or numbing gels, or talk to a sex therapist about the stop–start technique.
- Focus on enjoying sexual activity. Worrying about controlling your ejaculation may lead to erection problems or loss of interest in sex. Consider counselling to help ease your anxiety.
Difficulty reaching orgasm
If you’ve had your clitoris or other sensitive areas of the vulva removed, you may have difficulty reaching orgasm. Removal of the uterus, cervix and ovaries can also change how you experience sexual pleasure and orgasm.
Worrying about cancer or cancer treatment can make reaching an orgasm more difficult.
As the brain is one of the major sexual organs, thinking about past sexual experiences or fantasies can sometimes help. You could try exploring erotic stories in books, magazines or in film.
Tips for reaching orgasm
- Use masturbation to see what works for you.
- Use stroking and massage, or guide your partner’s hands or fingers to areas that arouse and excite you.
- Focus on your breathing. Try to tense and relax your vaginal and pelvic floor muscles in time with your breathing during penetration or while your
clitoris is being stroked. - Explore reaching orgasm without penetration. Try oral sex, masturbation with sex toys or all-over touching.
- Try different positions: experiment with tensing your thighs, closing or opening your legs or pointing your toes.
- Consider using an electric vibrator, which may give you the extra stimulation you need to reach orgasm.
Loss of sexual pleasure
During and after cancer treatment, some people find that even though they can still have sex, they don’t enjoy it as much. This may be for emotional reasons, such as worrying or self-consciousness, or from a physical cause, such as fatigue, nerve damage or painful intercourse. As side effects improve, many people start to enjoy sex again. If you had your breast or prostate removed, you may need to explore touch and stimulation to other parts of the body to feel ready for sex.
Tips for more enjoyable sex
- Consider agreeing to just touching, hugging and kissing. This is a chance to feel close to your partner and relax knowing there’s no expectation of sex.
- Choose a time when you won’t be disturbed, and set a calming peaceful atmosphere.
- Place your partner’s hands and fingers on the areas that arouse and excite you – or touch those areas yourself.
- Change your normal positions to more comfortable ones that increase stimulation.
- Try using a personal lubricant with a water base. Avoid warming gels or lubricants with perfumes or flavours added, which may irritate delicate tissue or sensitive areas.
- Accept that you may not reach orgasm every time. Take the pressure off by focusing on giving and receiving pleasure in different ways, not reaching a certain point.
- Learn mindfulness to help you stay in the moment with your partner. Listen to Cancer Council’s relaxation and meditation tracks, available in our Finding Calm During Cancer podcast series.
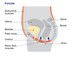
Changes to the vagina
Cancer treatments may cause temporary or permanent vaginal changes. Surgery may shorten the vagina, and pelvic radiation therapy can narrow the vagina, causing thinning of the walls and dryness. Penetration may become difficult and painful. A vaginal dilator may help.
Some people experience tight vaginal muscles (vaginismus) after cancer treatment. This is often caused by fear of painful penetration. Ask your health care team for a referral to a pelvic health physiotherapist, who can help you learn how to relax the pelvic muscles during penetration.
After cancer treatment, you may need vaginal moisturisers and lubricants to avoid discomfort during penetration.
Using vaginal dilators
A vaginal dilator can help keep your vagina open after treatment. A tube-shaped device made from plastic or silicone, the dilator is inserted into the vagina for short periods of time to gradually widen the entrance and prevent the walls sticking together. Dilators come in a range of sizes. You usually start with a short and thin one and “work up to” a longer, wider one over a period of time. It’s important to use dilators regularly for them to work. Vaginal dilators are not for everyone and they can be painful. If you don’t have penetrative sex, you may not worry about using one. Talk to your doctor about the benefits – for some people it’s worth it, and for others it may not be. Ask your health care team for a referral to a pelvic health physiotherapist. You can call Cancer Council 13 11 20 and ask to speak to someone who has used a vaginal dilator before.
How to cope with changes to the vagina
Some cancer treatments can change the size of the vagina and make sex uncomfortable or painful. A lack of oestrogen from some cancer treatments can cause vaginal dryness, which may lead to thrush. Treatments such as radiation therapy may cause a loss of sensation in the vagina.
Short/narrow vagina
- Use personal lubricant to make penetration comfortable. Choose a water-based or silicone-based gel without added perfumes or colouring.
- Ask your nurse or doctor about a non-hormonal vaginal moisturiser and apply several times a week to help keep your vagina lubricated.
- Try a vibrator or regular, gentle sexual intercourse. Experiment with positions for penetration.
- Use a foam ring around the base of your partner’s penis to reduce discomfort and pain during intercourse.
- Talk to your doctor about whether to use a vaginal dilator to widen your vagina after you’ve finished radiation therapy.
Vaginal dryness
- Avoid soap, bubble bath and creams that can irritate your genitals.
- Try a vaginal moisturiser. This non-hormonal, over-the-counter product can help restore lubrication and the natural pH level of the vagina and vulva. It is usually applied 2–3 times per week at night.
- Talk to your doctor about whether oestrogen creams or pessaries (tablets put into the vagina) are an option for you. They may not be right if you are having hormone therapy for cancer. Oestrogen creams are applied in the vagina or onto the vulva, and can help relieve discomfort.
- Personal lubricants are liquids or gels that are applied around the clitoris, labia and vaginal entrance, as well as your partner’s penis during sex. Try applying lubricant as part of your sexual foreplay. Lubricants with a silicone base may last longer than the water-based ones. Avoid oil or petroleum-based products (e.g. baby oil or Vaseline) as they can increase the chance of vaginal infection and damage latex condoms.
- To improve sexual arousal, take more time before and during penetration to help the vagina relax and become well lubricated.
Thrush
- Thrush can occur when genital dryness causes an overgrowth of a yeast-like fungus that is commonly found in the vagina. It can cause itching, burning and an unpleasant discharge, and may make intercourse painful.
- Seek medical advice to rule out other types of vaginal infections.
- Treat thrush with prescription creams or medicines.
- Wear loose, cotton clothes. Avoid nylon pantyhose, tight jeans or pants.
- Don’t use petroleum-based products (e.g. Vaseline) as a lubricant.
- Use a condom to avoid spreading thrush to your partner during sex.
- Ask a dietitian about what to eat to help control thrush. They may suggest eating foods low in sugar and yeast.
Loss of sensation
- Some women experience a loss of sensation in the vagina or labia which may be temporary or permanent, depending on the type of treatment they have had. This can make sex uncomfortable or unsatisfying, or may cause low libido and arousal.
- Focus on other areas of your body and genitals that feel pleasurable when touched.
- Try regular sexual activity of some kind to help maintain your interest in sex.
- Experiment with different sexual positions to try and find one that improves sensation.
- Use a vibrator to enhance sensation in the vagina and surrounding area.
- Seek medical advice – some women may benefit from a vaginal examination to identify and treat medical conditions such as thrush.
- If your usual contraceptive device or medicine is irritating you, try different types of contraception.
Pain
After surgery you may feel sore for several weeks, or longer in some cases. You may find it uncomfortable to be touched or hugged if the wounds from the surgery are still healing or if the area around the scar is painful. Pain can reduce your interest and pleasure in sex, and distract you from reaching orgasm. It may also mean the positions you used to have sex in are now uncomfortable. Some pain medicines may make you feel drowsy and tired, which may also affect your libido.
Painful intercourse
In the female body – Pelvic surgery, radiation therapy or treatment that affects hormones can reduce the size or moistness of the vagina, which can lead to painful intercourse. Some people experience vaginismus, when the muscles around the vagina tighten on penetration. This is an unconscious response and often caused by fear that intercourse will be painful. It’s important not to push on or persist through the pain as this can often makes things worse. Ask your health care team for a referral to a pelvic health physiotherapist. They can teach you how to keep your muscles relaxed during intercourse.
In the male body – Scar tissue in the penis after surgery can cause pain or bleeding, but it usually settles down in time. Irritation of the prostate or urethra from surgery or radiation therapy can cause painful orgasms. Anal sex can be painful after radiation treatment for prostate or anal cancer. Consider other ways to be intimate, such as oral sex.
Tips for managing pain
Managing pain during sex
- Plan sexual activity for the time of day when your pain is lowest. If you are using pain medicine, take it before sex (an hour before) so it will have maximum effect.
- Try different positions (such as side by side) until you find one that may be more comfortable for both of you and reduces pressure on painful areas.
- Use pillows or cushions to help you feel more comfortable and reduce pressure on a sore area.
- Try relaxation techniques such as a warm bath or massage before having sex.
- If pain continues, you can ask to be referred to a specialist pain clinic. It is important to deal with pain as early as possible, as a holistic approach is best for long-term benefits.
Making penetrative sex more comfortable
- Avoid deep pelvic thrusts – choose alternative positions where you can control the depth of penetration.
- Use plenty of lubricant. A water-based lubricant is easier to wash away but a silicone-based one will last longer. Talk to your health care team about which is best for you.
- Try to be close to orgasm or very aroused before penetration.
- Talk to a doctor or sex therapist if these methods don’t work. A women’s pelvic health physiotherapist may be able to advise on the use of vaginal
dilators and pelvic floor exercises to help manage painful intercourse. While using vaginal dilators can be challenging, they can usually offer improvement long-term. - Ask an occupational therapist what products can help with positioning during sex – they may suggest using wedges, pillows, electric beds or transfer boards.
- If pain is ongoing, ask to be referred to a specialist pain clinic.
Incontinence
Trouble controlling the flow of urine (urinary incontinence) or flow of faeces (faecal incontinence) is a common side effect of treatment for cancer of the prostate, bladder, bowel and penis, or of the female reproductive organs. Incontinence may be temporary or permanent. The pelvic floor muscles that affect bladder and bowel control also affect sexual function and arousal. Having bladder or bowel issues can be embarrassing and impact your sexuality, but there are ways to manage symptoms. For advice on incontinence, call the National Continence Helpline on 1800 33 00 66 or visit continence.org.au.
Tips for managing bladder and bowel issues
- Let your partner know that incontinence may occur.
- Cover your bed with large, fluffy towels or have sex in a wet area like the shower.
- If you have a catheter for draining urine, tape the tube to your skin, remove the bag and insert a flow valve or stopper before sex. For a catheter from a penis, fold the catheter back against the penis and put a condom on top to hold it in place.
- If you’ve had your prostate removed, try having sex in the missionary position with you on the bottom and your partner on top.
- Talk to a continence nurse about plugs for rectal use if you have faecal leakage.
- Learn how to exercise your pelvic floor muscles.
- Wait at least 2–3 hours after a meal, and empty both the bowel and bladder before having sex.
- Try positions that reduce pressure on the bladder such as being “on top”.
- See a pelvic health physiotherapist for advice. Ask your GP for a referral.
How to exercise your pelvic floor muscles
To identify your pelvic floor muscles, try stopping your urine stream for a couple of seconds while emptying your bladder. You use your pelvic floor
muscles to do this. Pelvic floor exercises should be done several times a day. The technique is the same for males and females.
- Start by relaxing all of your pelvic floor and tummy (abdominal) muscles.
- Gently lift your pelvic floor muscles up and hold while you continue breathing normally. Keep your upper abdominal muscles relaxed. Try to hold the contraction for up to 10 seconds. Relax your muscles slowly after each hold.
- Repeat the exercise up to 10 times, with a rest of 10–20 seconds between contractions. Relax your pelvic floor muscles completely during the rest periods.
Changes in appearance
If the way your body looks has changed after cancer treatment, you may feel self-conscious. It’s common to feel a range of emotions about the physical changes caused by treatment, which may include: changes to body functions; removal of a body part and use of a prosthesis, having a stoma; loss of hair from the head and body; weight loss or weight gain; skin rashes; swelling of part of the body (lymphoedema); and scars.
Some cancers of the head and neck can cause significant changes to what you look like, how you speak and how you eat or breathe. This can be upsetting because the change is visible, and kissing, speech and eating may be affected.
The way you look may affect how you feel about yourself. Changes to your face or body may make you feel less attractive, and this can affect your sexual confidence, self-esteem and body image. Often people find that their partner (or a potential partner) isn’t as concerned about these changes as they are. You may worry about other people’s reactions to you, or worry that they will avoid or reject you when they see how your body has changed.
It takes time to adjust to changes in appearance. Some physical changes may improve with time, while others may be more long-lasting. Focus on yourself as a whole person and not just the part that has changed.
Look Good Feel Better program
This free 2-hour program teaches adults and teens how to use skin care, hats and wigs to help restore appearance and self-esteem during and after treatment. Visit Look Good Feel Better to book into a workshop. They can also send you a confidence kit if you can’t attend in person.
Tips for adjusting to appearance changes
- Remember that sexual attraction is based on a mix of emotional and physical factors, not on a body part or physical characteristic.
- Look and touch your scars to get used to the changes.
- Use clothing, make-up or accessories that make you feel good or highlight your favourite features.
- Consider showing your partner any body changes before sex – and talk through what feels okay. Having your partner look at and touch these areas may help both of you get more comfortable with the changes.
- If you feel uncomfortable about a part of your body, you can wear clothes to cover it during sex – e.g. if you have had breast surgery you may choose to wear a camisole. You may also prefer to avoid sexual positions that leave the area exposed.
- Look at and touch your scars so you get used to the changes.
- Dim the lights or light candles when you have sex until you feel more confident about your body.
- If your hair has fallen out, you can wear a hat, wig or scarf, or you may prefer to leave your head uncovered. For more information, see Hair Loss.
- If you have concerns about weight loss or gain, choose well-fitting clothes. Something too tight or too baggy may highlight weight changes. Consider treating yourself to a new outfit that makes you feel comfortable.
- Ask your doctor about the possibility of plastic surgery or a facial prosthesis if surgery or radiation therapy has affected your face. This may help you regain a more natural appearance and help with any changes in the way you speak.
- See a counsellor to help you adjust to the changes.
Removal of a body part
If your cancer treatment involved the removal of a limb, breast or part of your genitals, it can cause feelings of grief, loss and anger. This can affect your sexual desire and your sexual confidence. It takes time to get used to how your body has changed and how that makes you feel. Try to remind yourself that you are loved for who you are, not for your particular body parts. Talking to a psychologist or counsellor may help you improve your sex life and relationship, and ease distress after surgery.
Breast – Nipple and breast sensation usually stay the same after breast conserving surgery, but may change after mastectomy. This can affect sexual arousal if you like being touched on the breast. The surgery may make you feel self-conscious or like you’ve lost a part of your identity.
Prostheses – People who’ve had a breast or testicle removed may use a prosthesis to improve self-esteem. This is a personal decision and not something everyone wants. Your specialist can give you more information about your options and what the procedure involves.
Anus – The removal of the anus is a major change, particularly if you have anal sex. It is a key erogenous zone for many people, and though some sex acts may not be possible, you can express intimacy through oral sex, cuddling and stroking. Penetration of the stoma (the opening created to remove waste after surgery) is not an option – it can cause serious physical harm and infections can be passed through the stoma.
Prostate – If the prostate is removed to treat prostate cancer, it can affect sexual pleasure when receiving anal penetration. For support, visit the Prostate Cancer Foundation of Australia and see Understanding prostate cancer for LGBTIQA+ people.
Tips for sex and intimacy after the removal of a body part
- Look at yourself naked in the mirror to get used to the changes to your body, or use a handheld mirror to see the genital area.
- Show your partner the changes. If it feels okay, teach them how to touch the area in a way that feels nice.
- Accept that it may take time to feel comfortable about your body again.
- If you have had one or both breasts removed, see ‘Breast Prostheses and Reconstruction‘ for more information.
- Touch your genitals to work out how your response has changed and what feels good. Explore other areas of your body that make you feel aroused when touched. This may take time and practice.
- If you are worried about the reaction of your partner (or a potential partner), remember that good communication will help. Sharing your concerns and keeping an open mind will help you explore new ways to be intimate.
- Ask your partner to stroke different areas of your body if your usual erogenous zone has been affected. This may include kissing and touching your neck, ears, inner thighs and genital area.
- If you’ve had a limb removed, try wearing your limb prosthesis during sex. If you prefer to take off the prosthesis, use pillows to support the affected limb.
- Call Cancer Council 13 11 20 to talk to someone neutral about your feelings.
- Register for a Look Good Feel Better workshop.
- Talk to a sexual health physician, psychosexual counsellor or sexual therapist about the ways any change to your body may be affecting your relationship and sex life. Visit the Society of Australian Sexologists to find an accredited sexologist near you.
Adapting to life with a stoma
Some types of surgery for bowel, anal or bladder cancer create a stoma – an opening in the abdomen that allows faeces (poo) or urine (pee or wee) to flow through and be collected in a small plastic bag. Sometimes a stoma is needed for only a short time, but in other cases it is permanent.
Having a stoma can affect your confidence and self-image, though a stoma often causes more embarrassment and distress to the person with a stoma than their partner. Getting used to looking after the stoma will help you feel more confident. Sexual activity for people with a stoma may need a little more planning but can still be satisfying and fulfilling.
Tips for sex if you have a stoma
- Change the bag and check the seal before having sex. This may help with worries about leaking.
- If you prefer, cover your bag with fabric or fold it in half and cover with a cummerbund to prevent the plastic clinging to your skin or the bag from flopping around. This can also help to keep it out of sight if that is a concern.
- Wear clothing that makes you feel good, such as a mini-slip, short nightgown or nightshirt, specially designed underwear or boxer shorts.
- Try sex in the bath/shower.
- After a heavy meal, wait for 2–3 hours before having sex.
- Talk to your stomal therapy nurse about learning irrigation to allow you to use a stoma cap or a small pouch (a “mini”) during sex.
- Use pouch deodorants or wear perfume to help control any odours.
- Allow your partner to see or touch the stoma.
- Contact a stoma association for support. Find one near you at the Australian Council of Stoma Associations Inc.
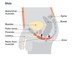
Adapting to life after a brain tumour
As brain tumours do not affect sexual organs, you may not expect sexuality to change. However the brain is responsible for sexual urges, thoughts and behaviours.
The areas most commonly involved in sexual functioning include the frontal, temporal and parietal lobe, and pituitary gland. When these parts are injured, it can cause problems with behaviour, thinking and memory, personality and social skills.
Possible changes in sexuality after a brain tumour include:
- loss of libido or sexual drive
- having an increased desire for sex (hypersexual)
- inability to achieve or maintain an erection
- difficulty or inability to orgasm
- premature ejaculation
- talking a lot about sex or inappropriate touching (disinhibition)
- weakness in an arm or leg, or slow and uncoordinated movements
- fatigue
- changes in self-image and relationships.
If you have become uninhibited or hypersexual after surgery, your family and friends may ask you to masturbate in private and not to make sexual comments. For help following brain cancer, call Cancer Council 13 11 20 or visit Building the Bridge to Life with Brain Cancer.
“The most distressing time for me was immediately post op when my side effects were many, varied and quite severe, even though most turned out to be temporary.” IAN
Early menopause
Natural menopause occurs when your ovaries stop working and you no longer menstruate (have periods). This means you will not be able to fall pregnant naturally. For most people, this usually happens between 45 and 55.
Most menopause symptoms are related to a drop in your body’s oestrogen levels. Symptoms may include aching joints, mood changes, hot flushes, night sweats, trouble sleeping, a dry vagina, reduced libido, dry or itchy skin, increased urinary frequency and “fuzzy” thinking. However, some people have few or minor symptoms.
Early menopause (premature ovarian insufficiency or POI) is the term for menopause that occurs before the age of 40. When this happens because of cancer treatment, it may be called induced menopause. When menopause starts suddenly, the symptoms are usually more severe than natural menopause because your body hasn’t had time to get used to the gradual loss of hormones. Premature menopause may also cause bones to weaken (called osteoporosis or osteopenia).
Going through menopause earlier than you expected may affect your sense of identity, or make you feel older than your age or friends. You may feel less feminine, and worry that you are not as attractive. For some people, not having periods is a positive.
Many kinds of cancer treatments can result in menopause symptoms or early menopause. These treatments include: surgery in which both of your ovaries are removed; hormone therapy to decrease your body’s production of oestrogen; and radiation therapy and chemotherapy, which may affect your ovaries’ ability to produce eggs and hormones.
If your uterus is removed (hysterectomy) you will no longer have monthly periods or be able to carry a child. However, if you still have at least one ovary, you will continue to produce oestrogen – which means you will go through natural menopause at the normal stage of life. If both of your ovaries and/or your uterus are removed, your periods will stop and you will experience a surgical menopause.
Tips for managing menopause symptoms
- If cancer treatment causes early menopause, consider seeing a menopause clinic to discuss the options for managing symptoms.
- Identify and avoid things that trigger hot flushes, such as alcohol, hot drinks, spicy foods or anxiety.
- Learn meditation and relaxation techniques, and exercise regularly to reduce stress and symptoms.
- Try topical hormone treatments, such as vaginal creams, to manage symptoms. There are also non-hormonal options, such as acupuncture.
- Talk to your doctor about the benefits and risks of menopause hormone therapy (MHT) for severe menopause symptoms.
- Ask your GP to arrange a bone density test to check for osteoporosis or osteopenia, which can develop after menopause.
- Try to eat high-calcium foods, talk to your doctor about a supplement, and exercise regularly to strengthen your bones and reduce bone loss. Call or visit Healthy Bones Australia on 1800 242 141.
Fertility issues
Some cancer treatments can cause infertility (difficulty conceiving a baby), which can be temporary or permanent. If fertility is important to you, talk to your doctor before your treatment starts about the risks and your options. It may be possible to store your eggs, embryos, ovarian tissue or sperm for use in the future.
When people learn that they may be permanently infertile, they often feel a great sense of loss. You may be devastated that you won’t have your own children or have more children, and you may worry about the impact of this on your relationships. Even if your family is complete or you didn’t want children, you may experience strong emotions. This can change how you feel about yourself as a sexual being and affect your sexuality.
As well as talking with your partner, it may help to talk with a counsellor, sex therapist, your GP or your cancer treatment team.
If female reproductive organs are affected – Surgery that removes part or all of the reproductive organs, such as the ovaries, fallopian tubes, uterus and cervix, will cause your periods to stop and you will be unable to conceive a child.
Depending on the type of chemotherapy drugs used and the dose, periods may become irregular but they often return after treatment ends. In some cases, periods stop permanently, leading to menopause.
If sperm production is affected – Surgery for bladder, prostate or testicular cancer may damage the nerves for getting and keeping an erection. This may be temporary, but some people may not get strong erections again, or have permanent erection issues. If the problem is ongoing, ask your doctor about collecting sperm.
Chemotherapy may reduce or stop sperm production and affect the ability of sperm to move. This can sometimes cause temporary or permanent infertility.
If you have radiation therapy in the pelvic or groin area, you may have temporary or permanent fertility problems after treatment. If your testicles are outside the treatment area, they can usually be protected. Radiation therapy to the brain may damage the pituitary gland, which affects both the production of sperm and sex drive.
Tips for managing fertility and treatment
- If you think you may want to have children in the future, discuss ways to preserve or protect your fertility with a fertility specialist before cancer treatment begins.
- Share your feelings about any fertility issues with your partner, who may also be worried or grieving.
- Ask your doctor what precautions to use during treatment. You may need to use barrier contraception, such as condoms or female condoms, to reduce any potential risk of the treatments harming a developing baby or being toxic to your partner.
- Tell your cancer specialist immediately if you or your partner become pregnant during treatment.
- Consider having tests to check if your fertility has been affected.
Featured resource
This information is reviewed by
This information was last reviewed August 2022 by the following expert content reviewers: Dr Margaret McGrath, Head of Discipline: Occupational Therapy, Sydney School of Health Sciences, The University of Sydney, NSW; Yvette Adams, Consumer; Dr Kimberley Allison, Out with Cancer study, Western Sydney University, NSW; Andreea Ardeleanu, Mental Health Accredited Social Worker, Cancer Counselling Service, Canberra Health Service, ACT; Kate Barber, 13 11 20 Consultant, Cancer Council Victoria; Dr Kerrie Clover, Senior Clinical Psychologist, Psycho-Oncology Service, Calvary Mater Newcastle, NSW; Maree Grier, Senior Clinical Psychologist, Royal Brisbane and Women’s Hospital, QLD; Mark Jenkin, Consumer; Bronwyn Jennings, Gynaecology Oncology Clinical Nurse Consultant, Mater Health, QLD; Dr Rosalie Power, Out with Cancer study, Western Sydney University, NSW; Dr Margaret Redelman OAM, Medical Practitioner and Clinical Psychosexual Therapist, Sydney, NSW; Kerry Santoro, Prostate Cancer Specialist Nurse Consultant, Southern Adelaide Local Health Network, SA; Simone Sheridan, Sexual Health Nurse Consultant, Sexual Health Services – Austin Health, Royal Talbot Rehabilitation Centre, VIC; Prof Jane Ussher, Chair, Women’s Heath Psychology and Chief Investigator, Out with Cancer study, Western Sydney University, NSW; Paula Watt, Clinical Psychologist, WOMEN Centre, WA.